Biomedical Business & Technology Contributing Editor
IRVINE, California — The U.S. healthcare system, by far the world's largest in terms of overall spending, is perennially criticized for excess cost, failure to deliver improved health status in spite of high levels of spending, gross inefficiency and high rates of uninsurance. While the deficiencies of the U.S. healthcare system represent a potential liability for politicians in both parties, recent attempts to improve the financing and delivery of healthcare in the U.S. have, with only a few exceptions, fallen short.
The annual Health Care Forecast Conference, organized here annually by the Paul Merage School of Business of the University of California Irvine, provides an insightful update on trends in politics and the economy and their impact on healthcare, as well as a critical assessment of new initiatives and policies aimed at fixing the defects of the healthcare system.
A significant development within the past year is new programs at the state level to overhaul healthcare financing, largely in response to a lack of any significant initiatives at the federal level. Authors of new healthcare plans in Massachusetts, California, and Florida discussed new programs that could radically alter the structure of healthcare in those states, and which are already being implemented in two cases.
The role of technology and process engineering in improving the healthcare system was another topic addressed at the conference, and it is a topic that has major implications for the medical device and diagnostics industries.
Market fundamentals defy policy solutions
A key component of healthcare costs — and a telling indicator as well for business and consumers — is trends in healthcare insurance premiums. In spite of initiatives at the federal level and by employers to shift the cost of healthcare to consumers and thereby make them more value-conscious in their utilization and purchase of services, insurance premiums have continued to rise at over three times the overall inflation rate, and three times the rate of increase in workers' earnings. While the rate of increase is down significantly from the double-digit rates that prevailed in the late 1990's and early 2000's, this is not considered to be a sustainable trend over the long term.
As shown in Table 1, the rate of increase in health insurance premiums, as well as the increase in healthcare costs, bottomed out in the mid-1990s, which not coincidentally coincided with the peak penetration in the U.S. of health maintenance organizations (HMOs). In addition, over the entire period from 1988 to 2006, the only years in which increases in insurance premiums were at or below the overall rate of inflation were 1995-1997.
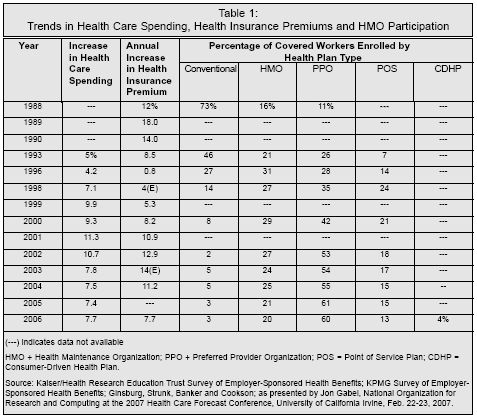 |
A consumer backlash against the restrictions of managed care rekindled healthcare cost inflation, however, and by 2002 the rate of increase again reached double-digit levels. Since then, due mainly to increased cost shifting from employers to employees, a trend to which employees responded by switching to higher deductible, less comprehensive coverage, premium increases have moderated.
But that has little to do with more price-conscious purchasing of healthcare services, since consumers' ability to compare prices and value in healthcare remains very limited. Instead, it reflects more out-of-pocket spending by consumers and, probably, some curbs on utilization.
Pushing other options
Consumer-driven health plans, while aggressively promoted by the federal government as a solution to rising healthcare costs, have so far had a minimal impact, since such plans accounted for only 4% of the market in 2006. Furthermore, many employees who enrolled in health plans that include Health Savings Accounts did so because some large employers made such plans the only option.
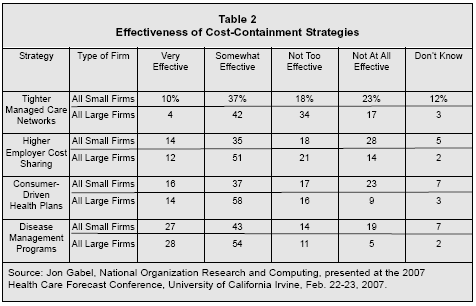
According to employer polls conducted in 2006, as described by Jon Gabel, senior fellow at the National Organization for Research and Computing at the University of Chicago (depicted in Table 2), disease management is considered to be the most effective cost-containment strategy, although consumer-driven health plans ranked second. Tighter managed care networks ranked last.
 |
As a further indicator of the declining role of managed care in containing healthcare costs, Kaiser Permanente (Oakland, California), the leading HMO with 8.7 million members nationwide, is moving away from the traditional HMO as the sole plan offered to its members. Instead, Kaiser is investing heavily in information technology, including electronic medical records (EMRs) and consumer IT networks, to improve efficiency and lower costs. This strategy also meshes with an increasing focus on disease management at Kaiser. In fact, Kaiser has now begun marketing its disease management programs to other healthcare providers.
Assessments of the effectiveness of disease management programs have produced evidence that outcomes are improved for chronic disease patients, but this evidence has not included proof that these programs save money or even pay for themselves. Consequently, slowing the rise in healthcare costs probably will require some new strategies.
Medicare Part D a culprit?
The federal government, for all of its pronouncements concerning the need to slow healthcare spending, has done little to accomplish this goal and may have exacerbated the problem with the passage of the Part D Medicare, prescription drug coverage for seniors. Part D is costing less than expected, however, because of low sign-up rates and low drug prices. And the program could conceivably provide a net cost savings if the federal government succeeds in negotiating significantly lower drug prices, reducing prices to a level at which the savings compared to drug purchasing by individual Medicare beneficiaries exceed the costs of administration.
However, as discussed by Andie King, former domestic policy advisor to Democratic leader Richard Gephardt, most observers expect the Part D program to add to healthcare costs as drug utilization by seniors grows, resulting in an increase in the budget deficit. And there is scant hope for major changes this year, according to King and other presenters discussing short-term policy at the federal level. These included Elizabeth Fowler, PhD, VP of public policy and external affairs at Wellpoint (Indianapolis), and former chief health counsel, Senate Finance Committee; Dean Rosen, MD, a partner at Mehlman Vogel Castagnetti (Washington) and former health policy director for Senate majority leader William Frist, MD; and Norman Ornstein, PhD, resident scholar, American Enterprise Institute (Washington).
This inactivity stems from the offsetting balance of power between the newly elected Democrat-controlled Congress and the Republican administration, with President Bush retaining a little-used veto as a barrier to passage of any new congressional legislation.
An additional factor hampering the passage of new legislation, and of rescinding any initiatives that would cut healthcare spending at the federal level, is the PAYGO policy adopted by House Democrats. PAYGO requires that any new spending programs be accompanied by offsetting budget cuts in other programs, and that cuts that have already been authorized — such as the rollback in Medicare fees for imaging services in physician-owned centers implemented in January 2007 and savings from competitive bidding programs implemented for laboratories, not be rescinded unless corresponding cutbacks are implemented in other programs.
The overall environment makes passage of any new legislation extremely difficult, even though the newly elected Democrats will want to show that they can produce results in contrast to the Congress it replaced and which they characterized as do-nothing.
Experts such as Ornstein say there is pent-up demand in the country for action on healthcare issues, heretofore crowded out by the war in Iraq.
States acting where feds don't
Some states have responded to Washington's inertia on healthcare by proposing and implementing new programs of their own.
At the conference Cindy Gillespie, counselor to former Massachusetts governor and presidential candidate Mitt Romney, described the state's newly implemented healthcare plan mandating universal healthcare. Key characteristics of the program include an Insurance Connector that mates insurers such as Blue Cross/Blue Shield and various employer-funded health plans with individuals and small businesses to allow insurance to be purchased with pre-tax dollars regardless of employment status. This makes healthcare insurance entirely portable and allows insurers to offer plans with higher deductibles consistent with Health Savings Accounts.
The program provides free insurance for persons below the Federal Poverty Level ($9,800 for single persons), and progressively higher rates for those with higher incomes, ranging up to $106 per month for a single person making $29,400 (300% of the poverty level).
The plan requires that everyone be insured or have the means to pay for their own healthcare, a mandate that has proven controversial, primarily because that feature eliminates the $1.3 billion in spending by the state on free care previously provided to the state's 460,000 uninsured by "safety net" hospitals, largely via expensive emergency room care, replacing it with $980 million in spending on premium assistance provided by the new health plan.
The program has the added advantage of pulling additional young, healthy individuals into the insurance risk pool and of reducing the hidden tax on employers and self-insured individuals who provide health insurance and previously subsidized free care.
The California initiative
California's new Health Care Initiative program proposed by Governor Arnold Schwarzenegger was described by Ruth Liu, one of the plan's architects. She noted that the scale of the problem of the uninsured in California is considerably different than in Massachusetts, with a total uninsured population estimated at 6.5 million, or about 18% of the state's population.
About 84% of the uninsured in California are employed, and 66% are full-time employees. Furthermore, unlike Massachusetts, there is no designated safety net pool of funds to cover the cost of free care provided to the uninsured.
According to data from the New America Foundation (Washington), families in California pay an average of $1,186 annually in hidden tax in the form of 10% higher health insurance premiums to cover the cost of care for the uninsured, and individuals pay $455 per year.
The California program not only addresses coverage of the uninsured, but it is also designed to reduce the hidden tax and thereby lower insurance costs across the board; and it also provides incentives for disease prevention and wellness programs, further enhancing the long-term affordability of the initiative. Specific areas targeted for prevention and wellness include diabetes prevention and treatment, reduction of medical errors (via e-prescribing and stronger patient safety programs), obesity prevention and smoking cessation.
As in Massachusetts, the proposed program would include an individual mandate to have health insurance coverage, since requiring only employers to provide coverage would not reach all of the uninsured. Other features include automatic coverage of children under the State Children's Health Insurance Program (SCHIP) for all families making under $60,000 per year (for both documented and undocumented workers); a 2% fee levied on physicians and a 4% fee for hospitals; and a requirement that insurers offering plans in the state spend 85% of the premiums they receive on patient care.
The approach in Florida
Also described at the UCI conference by Alan Levine, president/CEO of the North Broward Hospital District and former secretary of health for the State of Florida, was that state's somewhat different approach.
After evaluating the Massachusetts plan, Florida concluded that it was unaffordable because of the much larger number of uninsured persons (4 million), representing about 22% of the population vs. about 7% in Massachusetts.
According to Levine, the large proportion of uninsured is characteristic of immigrant destination states such as California, Texas, and Florida. Furthermore, according to Levine, a program that only addresses the uninsured does not solve healthcare's more fundamental problems. Instead, Florida has implemented programs to improve the efficiency and cost-effectiveness of healthcare, including incentives for insurers to implement or fund preventive care and chronic disease management programs through risk-adjusted payments from the state’s Medicaid program.
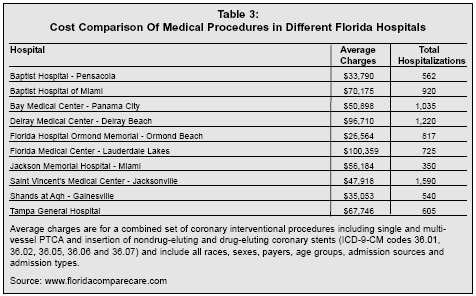
Another initiative — this one implemented by repeal of a law that prevented public disclosure of hospital outcomes data — is improved transparency of the healthcare delivery system. The state has implemented a website, www.FloridaCompareCare.com, which provides comprehensive data on procedure volume, cost and length of stay for all hospitals in the state, allowing consumers to compare healthcare costs and quality.
Table 3 presents a sampling of data from the site that shows the wide disparity in cost for the same set of procedures performed in different hospitals. The site also provides data on ambulatory surgery centers and pharmaceutical pricing.
 |
While the new state initiatives may provide important indicators concerning the future direction of U.S. healthcare, several conference presenters noted previous healthcare reform efforts by several states, including Oregon, Hawaii, Tennessee, New York, Vermont, Oklahoma, Delaware and Wisconsin. Most of those programs have encountered difficulties due to budget issues, they noted, predicting similar hurdles for the new programs. For example, Lieu said that California's proposed initiative will cost a cool $12 billion.
Economic growth forestalls difficult choices
This is a bad news/good news story because to some extent, the continued growth of the U.S. economy, along with low levels of unemployment and, most recently, rising wages, has helped to blunt the demand for healthcare reform. From a global perspective, healthcare spending is tied in a non-linear fashion to gross domestic product, and as long as the U.S. economy continues to expand, the wherewithal exists to support some healthcare cost increases.
As discussed at the conference by James Glassman, PhD, senior economist and managing director, JP Morgan Chase & Co. (New York), the health of the economy is no longer the business community's major concern. It is focusing, instead, on issues such as fairness.
Changes in credit policy and the international transfer of capital have made the U.S. economy more resilient, and growth in productivity, coupled with outsourcing of labor, has fueled economic expansion while putting a brake on inflation.
Another key factor creating momentum for continued economic growth is the general expansion of international economies. The living standards in China and India have increased from 5% of that in the U.S. in the mid-1970s to 10% today, and could reach the level in the U.S. by 2050, according to Glassman.
The U.S. trade deficit, an oft-cited indicator of economic weakness, is helping to fuel growth in the developing countries, while creating new long-run market opportunities for U.S. firms — especially in the healthcare and medical device sectors. This benefit will begin to become more obvious as trade deficits start to shrink, as they are now with Europe, and are trending in that direction with China.
Medicare/Medicaid on the rise
Federal fiscal health also plays an important role in the U.S. healthcare system, since government-funded Medicare, Medicaid, and SCHIP programs account for more than 30% of U.S. healthcare spending, or 4.8% of GDP in 2002.
According to James Baumgardner, PhD, deputy assistant director for health policy at the Congressional Budget Office, total federal spending for Medicare and Medicaid could climb to 21.3% of GDP by 2050, using an assumed excess cost growth (of per-capita healthcare spending vs. per-capita GDP) of 2.5%, slightly lower than the historical average. The entire federal budget currently consumes about 20% of GDP.
Put in other terms, according to Robert Berenson, MD, senior fellow, The Urban Institute (Washington), by financing the projected deficit in Medicare spending through 2080, Medicare's payroll tax rate would need to increase immediately from 2.9% to 6.4%. Or health spending would need to decrease 51%.
Nevertheless, Baumgardner said, the federal budget picture is reasonably bright for at least the next 10 years. As shown in Table 4, the actual deficit in 2006 was just under $250 billion, or 1.9% of GDP, which was less than projected a year ago due to higher-than-expected federal revenues and per capita Medicare spending that was less than forecast.
 |
As noted, costs for the new Part D Medicare prescription drug program were also less than expected due to lower per-capita costs than forecast. The Congressional Budget Office now projects a surplus beginning in 2012, though that assumption depends on an expiration of certain tax provisions that may or may not occur. In addition, beginning in 2011, when the baby boom generation begins to turn 65, current assumptions may become invalid, and federal spending on healthcare could come under increasing pressure.
Impact of technology, process re-engineering
One healthcare development which all presenters at the UCI conference agreed on will move forward is the implementation of information technology (IT) as a way to solve healthcare delivery inefficiencies.
At present, as discussed by Arnold Milstein, MD, MPH, chief physician, Mercer Human Resource Consulting (New York), and medical director, Pacific Business Group on Health (San Francisco), healthcare is in a pre-automation stage and healthcare service consumers want systems that operate more like today's high-efficiency businesses.
According to Milstein, more than 50% of healthcare costs are due to waste and inefficiency within the delivery system, an issue that can be addressed by implementing IT solutions and process re-engineering methods proven in industries such as financial services, retail sales and the automotive industry.
One metric cited by Milstein is the time required to implement new approaches into medical practice — which he put at 17 years — compared to six months in the semiconductor industry. And he said that adoption of best practices employed in other industries could provide other major savings.
One reason such advances have not occurred to date is that most physicians and healthcare staff lack process engineering backgrounds, a deficiency being addressed by purchasers of healthcare services, particularly large employers with self-funded insurance plans that also have strengths in process engineering. These companies are now offering assistance in process redesign to healthcare providers to improve efficiency and lower costs.
Focus: the 20/60 rule for improvement
Milstein said that the main focus of efforts for improving efficiency should be, at least initially, on the sickest 20% of patients who account for about 60% of spending. One approach to better efficiency, comprised of strategies already implemented and validated by leading experts in process efficiency, is the ambulatory ICU, which focuses on improved structures for delivery of primary care to the sickest 20%. The overall strategy involves a greater reliance on disease self-management enabled by economical relationship-based coaching, coupled with lean primary care MD visits, and referral to the most cost-effective specialists and hospitals.
While the cost of implementing and managing such a strategy would increase spending by 13%, the savings from improved efficiency at all levels is estimated at 48%, and results in 35% lower net spending.
That strategy includes use of new technologies such as remote monitoring to assist patients in compliance with self-improvement plans. Significant improvements in efficiency for management of the sickest 20% of patients — based on a projected 35% savings for that population — would produce a 20% reduction in total healthcare spending.
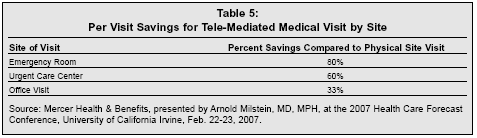
Milstein proposed addressing the low efficiency of healthcare provided to the remaining 80% of patients through use of technologies such as video visit booths in pharmacies that would link them to tele-mediated care. The booths would operate 24 hours a day, and would be staffed by on-site paramedics or pharmacy technicians to conduct an initial medical evaluation based on MD-set clinical protocols, to include medical history, biometric data, a limited physical exam, and instant point-of-care labs and ECG measurements.
A physician provides a remote consult by viewing the data and interacting with the patient, and then either recommending a treatment plan or requesting more data collection. The patient then either fills a prescription at the pharmacy if necessary, and/or receives referral to the most cost-effective and accessible care.
According to an analysis by Mercer Health, this approach could drive substantial savings compared to existing approaches such as office visits, visits to urgent care centers, or emergency room visits, as shown in Table 5. The technologies needed to implement such an approach already exist, but barriers to widespread adoption include a lack of recognition of inefficiencies of the existing healthcare system, the vested interests of healthcare providers, and the capital required to implement such a system.
 |
EMRs a necessity
EMRs could also figure prominently in the equation for improved healthcare efficiency and cost reduction. Though the actual return on investment remains to be demonstrated, there is clear movement toward the use of EMRs in the U.S. and other developed countries.
Sheldon Greenfield, MD, director of the UCI Center for Health Policy Research, discussed new technologies such as the Colorado Care Tablet, a tablet personal computer that is based on the paper personal health record but automates collection of patient data and can facilitate coaching of patients to allow them to better manage their disease. The computerization of healthcare has been slowed by the need to convince physicians to adopt it, but that may be changing as Generation Y physicians, who have used computer technology since childhood, begin to enter medical practice.
Other advanced technologies that allow a shift in care settings, discussed by Mary Kate Scott, senior advisor for HealthTech (San Francisco), include tele-ICUs, advanced imaging systems, the electronic ICU, digitized pathology, and on-line patient safety.
New delivery paradigms
An example is the eICU developed by Visicu (Baltimore), which employs a remote intensivist-led care team to monitor hundreds of ICU patients in real time through computerized links, providing constant surveillance and immediate physician access for every patient. Addressing the shortage of intensivists in existing ICU's, the Visicu system is designed both to reduce costs and to reduce mortality by 25%.
Another new development changing the paradigm of primary care is the rapidly growing network of rapid-service, low-cost clinics being established nationwide by companies such as MinuteClinic (Minneapolis). The number of such clinics, typically found in supermarkets or pharmacies such as CVS (Woonsocket, Rhode Island), grew from 60 to 255 in one year and are projected to increase to more than 500 this year and to 800 by 2008, according to Scott.
Rapid, low-cost primary care is being enabled by advances in point-of-care diagnostics, such as rapid lipid profiling systems from Cholestech (Hayward, California) and similar CLIA-waived diagnostic devices.
Another new technology designed to improve the efficiency and efficacy of the healthcare process described by Scott is the web-based healthcare communications system developed by Emmi Solutions (Chicago), used by providers to educate patients about medical procedures and guide them through the treatment and recovery process.
The system uses advanced video animation to present patient care and patient safety methods.
In the hospital setting, examples of new technologies to enhance efficiency include the Awarix patient care visibility system from Awarix (Birmingham, Alabama). The system employs RFID and ultrasound to track patients throughout the hospital, presenting patient status on electronic whiteboards that allow patient tracking and assessment on large-screen displays, thus intended to improve the efficiency of patient management in the hospital, while maximizing utilization of beds and other resources.
