BBI Contributing Editor
CHICAGO, Illinois The American College of Surgeons (ACS; Chicago) held its 89th annual clinical congress here last fall under near-record high temperatures. Since general surgeons perform a variety of procedures and can cross over into several sub-specialties, topics ranged from A to Z, or in surgical terms, from bariatric surgery to vascular surgery. Treatment of these two diseases is no longer viewed as cosmetic procedures real health risks have been associated with both obesity and varicose veins and are now being approached as serious health problems.
As an indicator of how varied a general surgeon's practice is, it should be noted that of the top 10 diagnoses seen in office visits, not a single diagnosis makes up even 10% of a surgeon's daily practice.
In one of the more popular general sessions at the ACS meeting in the lakefront McCormick Place convention center, a panel of experts debated the pros and cons of current issues in a discussion of "New Technology: What's Proven, What's Not," and, using an audience interactive response system, allowed the audience to vote on the "winner" of each debate.
One debatable topic was that of bariatric surgery. In a session titled "Bariatric Surgery Is Procedure of Choice and Should Be Offered to Almost All Suitable Patients with Morbid Obesity," Henry Buchwald, MD, professor of the department of surgery at the University of Minnesota (Minneapolis, Minnesota), took the "pro" position and said that there are no drugs, behavior modifications or combination programs that work long-term and that surgery is the only option for a successful outcome for this patient population. Obesity is currently the second-leading cause of death in the U.S. next to smoking. Potential candidates for bariatric surgery must have a body mass index (BMI) of over 35, along with the presence of co-morbidities. Buchwald, who has performed more than 2,000 bariatric procedures, maintained that only bariatric surgery would eliminate the co-morbidities that accompany morbid obesity (see Table 10.)

Although there have been a variety of surgeries to correct obesity since gastric stapling in 1977, not until 1994, with the Roux-en-Y gastric bypass developed by Alan Wittgrove, MD, and G. Wesley Clark, MD, of the Alvarado Center for Surgical Weight Control (San Diego, California), did surgical procedures for obesity become popular, growing by 300% since 2001, with 40,000 procedures in that year, 86,000 in 2002 and an estimated 120,000 in 2003.
Bariatric procedures advance
Buchwald outlined four basic types of bariatric procedures (see Table 11 below), some aimed at restriction of the stomach capacity, some that induce degrees of malabsorption by bypassing part of the small bowel, or some that are a combination of the two. All of the surgeries can be performed via open or laparoscopic techniques.
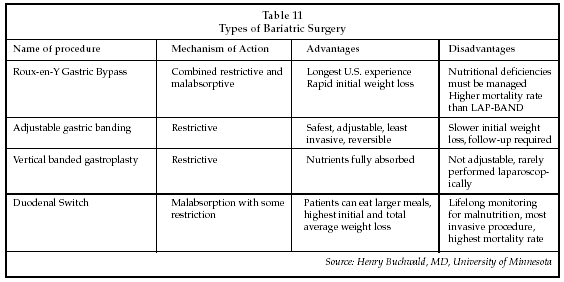
He said that the most commonly performed bariatric procedures are the laparoscopic Roux-en-Y (gastric bypass) and the adjustable laparoscopic gastric band (LAP BAND) marketed by Inamed Health (Santa Barbara, California). The LAP BAND procedure is currently growing the most quickly in the U.S., in part due to a shorter learning curve for surgeons. Recent studies have shown that the LAP BAND takes about 75 cases to be "up the learning curve," while the Roux-en-Y takes closer to 150 cases.
Buchwald reviewed 16 papers that included more than 4,000 patients that had the adjustable gastric band procedure and their average weight loss at two years was 50% of the excess weight. He also reviewed 20 papers that included more than 3,300 patients having had the Roux-en-Y procedure and found on average a 70% excess weight loss. Both results showed a complete reversal or significant reduction in all co-morbidities, including resolution of 90% of all Type 2 diabetes, and resolution of hypertension and sleep apnea in excess of 50% of cases. The American Society for Bariatric Surgery (Gainesville, Florida) has tracked an average weight loss from bariatric procedures of more than 50% of excess body weight maintained 16 to 18 years following surgery.
Privately held, venture-funded Satiety (Palo Alto, California) takes a decidedly different route to helping solve the obesity puzzle. The development-stage firm offers what President and Chief Executive Officer Matthew Collier describes as a "very different solution" to obesity that offers a "quick, low-risk outpatient procedure" that stands in contrast to "very risky surgeries."
Satiety's technology takes stomach "restriction" inside the organ, conducted by a flexible endoscope. The non-surgical procedure is done under conscious sedation, with the endoscope inserted through the throat to staple together a small segment of the stomach, thus restricting intake. It involves a relatively minimal level of additional skill by a physician conducting it, greatly expanding the potential number who can carry it out beyond the fewer than 2,000 estimated to be trained to conduct gastric bypass procedures.
Despite the fact that cost analysis studies have shown that the annual cost of treating a morbidly obese patient is more without the bariatric surgery than after surgery, most insurance companies do not cover such procedures. In addition, one study found that 16% of bariatric surgeries cost more than forecasted, usually due to apnea or hypertension following surgery that required additional hospital time. But patients are willing to pay the $15,000 to $25,000 it costs to improve their health, quality of life, and their longevity.
Buchwald also noted that the gastric pacemaker manufactured by Transneuronix (Mt. Arlington, New Jersey) is still considered developmental, although more than 400 implantable gastric stimulators have been placed in patients worldwide. This device does not change the anatomy, is surgically placed in the stomach using a minimally invasive procedure and appears to be effective, although the mechanism of action is not clearly understood yet.
Walter Pories, MD, professor of surgery at East Carolina School of Medicine (Greenville, North Carolina), was assigned to the "con" side of this debate and had only one argument, that being for standardization of bariatric procedures. He showed dozens of various bariatric procedures and said that even performing the standard Roux-en-Y, there were many variances from pouch size to length of bypass. Pories said that by not standardizing the procedures, the learning curve for the profession is not being advanced. Clinical studies cannot be trusted with multiple surgeons, much less multiple sites, with each performing their own method of surgery, he said. One promising aspect of the adjustable lap band, he said, is that the surgery is standardized; only the adjustments post-surgery are customized to the patient. The audience vote was 65% for bariatric surgery as the procedure of choice for morbidly obese patients.
New focus on venous vascular surgery
A subspecialty of general surgery that is receiving much attention lately is that of vascular surgery, and venous vascular surgery in particular. Like all surgical specialties, vascular surgery is struggling with poor reimbursement, increasing malpractice premiums, increasing overhead and more complex procedures to perform for the same amount of reimbursement. In addition to these maladies, the vascular surgeon is finding himself entangled in a battle for patients. Historically, vascular surgeons were a subspecialty of general surgery with a special certification that permitted them to operate on all vessels arterial or venous outside of the heart. As less-invasive, catheter-based procedures started to become the norm for treating many of the vascular diseases, the vascular surgeon found himself competing with interventional radiologists and interventional cardiologists for the same patient. Because of this, some surgeons are now seeking procedures that do not compete with other specialists, such as venous procedures. Recently, less-invasive methods of vein care have required greater technical skill, providing for higher reimbursement levels and, most importantly, patient demand for these procedures. Surgeons are becoming more interested in performing minimally invasive venous procedures to increase revenues without having to compete for the patient, as well as filling the demand created by a larger patient pool.
Peripheral vascular surgery has been growing for clinical reasons as well. Varicose veins have been proven to be a symptom of an underlying disease process that needs to be treated. Vascular disease attacks all vessels and is an ongoing process. Since the coronary arteries are the smallest, they occlude the earliest and are treated first. Prior to advances in cardiovascular medicine, patients died of heart attacks before their peripheral vascular disease was detected. Now that their hearts are being treated, they are living long enough for the disease process to become symptomatic in other vasculature of the body. New technology is another driver for increased peripheral vascular procedures. When such procedures required open surgery accompanied by high risk and high cost, the patient often was not put at that risk and merely given palliative therapies. Now that minimally invasive, safer procedures are available with associated lower cost, more patients are seeking treatment for their peripheral disease (Table 12).

It is estimated that 20% to 40% of all Americans have some form of venous insufficiency, and 25 million Americans suffer from symptoms associated with superficial venous reflux and varicose veins. The venous system of the legs consists of the deep venous system, the superficial vein system, and the perforator vein system, with each system having its own specific method of treatment (Table 13). Endovenous treatments may be office-based, done under local anesthesia and last about 45 minutes. The Closure procedure developed by VNUS Medical Technologies (San Jose, California) usually is performed on an outpatient basis under either local or regional anesthesia. The SEPS procedure, which is the only one addressing perforator veins, is usually an outpatient procedure done under general or regional anesthesia. All have nominal recovery time.

Approved by the FDA in 1999, the Closure procedure has been performed in more than 35,000 greater saphenous vein procedures, reporting 94% of their patients reflux-free at four years. VNUS' technology is an endovenous approach that occludes veins using radiofrequency energy, thereby eliminating reflux. In a similar fashion, but using laser energy instead of RF energy, Diomed (Andover, Massachusetts), Dornier Medtech (Kennesaw, Georgia) and AngioDynamics (Queensbury, New York) have performed about 10,000 procedures with a greater than 60% success rate since their approvals in 2002.
U.S. Surgical (Norwalk, Connecticut), a unit of Tyco Healthcare (Exeter, New Hampshire), has developed a set of instruments for subfascial endoscopic perforator surgery (SEPS) consisting of a balloon dilator that greatly facilitates the creation of an optimal subfascial working space, is cost-effective and offers a straight-forward refinement to the technique. The SEPS procedure is an effective method to treat patients with complications from chronic venous insufficiency.
These minimally invasive methods of treating symptoms associated with superficial venous reflux and varicose veins should help the 25 million Americans suffering from this disease.
