BB&T Contributing Writer
LAS VEGAS — More than 1,500 of the 3,200 members of the American Association of Gynecologic Laparoscopists (AAGL; Cypress, California) attended the Global Congress of Minimally Invasive Gynecology meeting here in November. Topics of interest spanned several areas that were once newly emerging technologies. For the most part these technologies were presented first at this conference only a few years ago but now have gained traction in community-based practices. This is especially true for procedures — such as treatment for fibroids and intrafallopian tubal occlusion for permanent sterilization — that were once performed in the hospital but can now be performed in an office setting.
In a postgraduate course Daniel Breitkopf, MD, of the University of Texas Medical Branch (Galveston, Texas) presented "An Overview of Hysteroscopic Tubal Occlusion Techniques — What is Available Now and What is Coming in the Future." He began with a reminder of the brief failed histories of hysteroscopic, as opposed to laparoscopic, tubal occlusion technologies, which began in 1934 with electro-coagulation of the tubes, followed by IUD insertion of quinacrine pellets in 1970, and then silicone plugs in 1983. Finally, in 2002, the Conceptus Essure device was cleared by the FDA.
By show of hands, about 40% of those attending the course indicated they had placed at least one Essure device. The Essure device consists of two nitinol micro-inserts containing a Dacron implant that promotes tissue ingrowth and is placed using a proprietary transcervical insertion instrument.
"The success of all intrafallopian tubal occlusion devices is in the tissue ingrowth following placement of the device, not in the occlusion of the insert itself. It is the tissue in-growth that blocks the tubes," Breitkopf said. He said that "the current Essure success rate of bilateral placement is 98%, the procedure takes on average 36 minutes total, 13 minutes for the placement itself, and boasts a 99.95% effectiveness rate. The procedure can be done in an office setting without IV sedation and is often cost-favorable to a laparoscopic tubal ligation.
But he then asked: "Why, then, aren't more patients electing an intrafallopian tubal occlusion over a laparoscopic tubal ligation?"
He said one reason often given is that patients are not willing to undergo the hysterosalpingogram (HSG) procedure that is required as a follow-up for the Essure placement. As a way to remove that bias, Breitkopf referred to a survey performed in Britain where no follow-up HSG is required and where eligible patients were given a choice between the two procedures. Slightly more than 75% of the patients chose a laparoscopic tubal ligation.
Patient reasons for the choice of permanent sterilization include the desire of immediate results, the rapidity of the procedure, the lack of scars, quicker recovery and the desire not to have something left in the body.
Breitkopf then discussed the other intrafallopian devices currently being developed, listed in Table 3.
 |
With the market adoption of the Essure system now robust and annual revenues running at about $40 million, it appears that any major player in the gynecology space now needs to incorporate a transcervical sterilization product. Other than the women having their last child and selecting same-time permanent sterilization immediately following birth, many women are predicted to select an in-office permanent sterilization procedure now that reimbursement is in place, rather than a laparoscopic tubal ligation that entails hospitalization.
Dealing with fibroids
Less-invasive techniques for the removal of fibroids — especially if they are designed to maintain the woman's fertility — continue to storm the marketplace. The removal of fibroids, termed a myomectomy, can be a technically challenging surgical procedure. And because many of the patients presenting with fibroids wish to maintain their fertility, it becomes even more challenging to avoid adhesions or compromise the uterus in any way. Table 4 outlines the many novel approaches discussed or exhibited at the conference that provide for less invasive or non-invasive technologies to ablate fibroid tumor. Most of these also enable treating the patient in a less intense setting than an operating room.
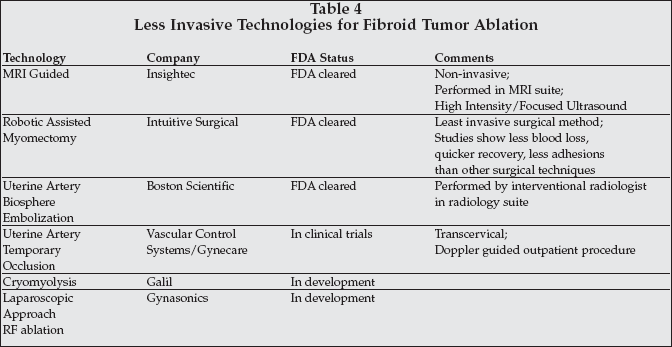 |
Robotic surgery by Intuitive Surgical (Santa Barbara, California) and MRI-Guided High Frequency Ultrasound (HIFU) from Insightec (Dallas) peppered the podium and poster presentations, as well as engaging a significant share of exhibit action. Insightec has developed and marketed an MRI-guided HIFU system FDA-cleared for non-invasive ablation of fibroids. And the company was offering clinicians the opportunity to witness live HIFU procedures for fibroid ablation at the local office that had just recently purchased the 36th system sold.
C.J. Ascher-Walsh, MD, of the Sinai School of Medicine (New York), presented "Robot-Assisted Laparoscopic Myomectomy Represents an Improvement Over Standard Laparotomy for Patients with a Limited Number of Fibroids" in which she compared the effects of the robotic surgery versus standard laparoscopic surgery on procedure time, length of stay, transfusions, charges, reimbursement, nursing, pharmacy, depreciation of the robot, and other pertinent factors. She found that "when everything was considered [for myomectomies] the robot became cost-effective and offered an improvement to the care of women with a small number of myomas."
Bryan D. Cowan, MD, professor and chair of the Department of OB/Gyn, University of Mississippi (Jackson), presented two clinical studies that he had performed using a new cryoablation device from Galil (Yokneam, Israel) for cryomyolysis, or freezing of the fibroids, with the intent to shrink them. In his series of 12 patients in each study — one group treated using MRI guidance, the other a laparoscopic cryoprobe — he showed a 50% reduction in fibroid volume at three months and 87% reduction in fibroid volume at six months, with 10 of the 12 patients having symptom improvement. He acknowledged the higher cost of the MRI but added that with laparoscopic or even ultrasound guidance he "anticipated a less-expensive price than many of the other emerging technologies for fibroid removal or ablation."
George Vilos, MD, professor of obstetrics and gynecology, The University of Western Ontario (London), presented "Transvaginal Doppler-Guided Temporary Uterine Artery Occlusion for the Treatment of Symptomatic Fibroids" in which he studied the feasibility, safety and efficacy of the Flostat system, now owned by Gynecare/Ethicon (New Brunswick, New Jersey). He studied 30 women who had their uterine arteries clamped for six to nine hours and found significant reduction in menorrhagia and a reduction in uterine and fibroid volume at six months. He concluded that "temporary uterine artery occlusion provides the gynecologist with an alternative to uterine artery embolization. The system is simple and easy to apply with the efficacy equivalent to UAE"
Although many of the emerging fibroid treatments are not yet out of the operating suite at this time, the movement is to a less-intense setting and some will eventually make it into an office based setting.
The No. 1 reason cited by gynecologists for their desire to move a procedure into an office setting was that the number of procedures accepted by patients increased significantly when the procedure could be performed in an office setting rather than a hospital. The second reason for wanting to move a procedure into the office was to generate greater revenue and maximize efficiency.
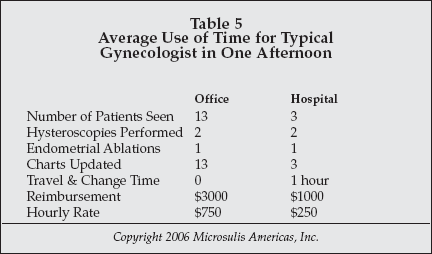
Microsulis Americas (Waltham, Massachusetts), manufacturer of a microwave endometrial ablation system designed for office use, studied office practices in the U.S. and found that the clinician could make better use of his time by performing procedures in the office, as shown in Table 5.
 |
