BB&T Contributing Editor
NEW ORLEANS — The Obesity Society (Silver Spring, Maryland), formerly known as the North American Association for the Study of Obesity, drew an attendee group of 2,200 researchers, clinicians, physicians, nurses, dieticians and behavioral scientists to its late-October annual meeting at the Ernest N. Morial Convention Center here.
This conference is certain to grow both in attendance and general interest given the increasing seriousness of the problem of obesity, its presence as a risk factor for a variety of diseases and, perhaps most significantly, the financial opportunity the problem offers for medical technology.
It is a worldwide problem most obviously seen in developed countries. Among these, the U.S. is the rather large, fat canary not in the coal mine, but in a large room of the over-adiposed. The prevalence of obesity in the U.S. has increased from 12% in 1962 to about half of the present population. An estimated 23 million people in the U.S. have a body mass index (BMI) of no less than 35kg/m2 and 8 million have a BMI of 40 kg/m2 or higher.
Globally, the statistics also are staggering, with some 2 billion people documented as overweight (25 to 29 kg/m2) which ironically, and suggesting a serious worldwide maldistribution of resources approximates the number of people that are starving worldwide.
According to the Centers for Disease Control and Prevention (Atlanta), 66% of the U.S. adult population, or 200 million people, are overweight or obese. The most recent National Health and Nutrition Examination Survey (NHANES) shows that the portion of the population which is obese has increased from 23% in 1988-94 to 32% in 2003-2004 and that 17% of children and adolescents (2 to 19 years old), or 12.5 million people, were overweight. Also, about 5% of adults, or 15 million people, are 100 pounds or more overweight. It is estimated that by 2015, 75% of all adults will be overweight or obese, and 14% will be obese.
The American Society for Metabolic & Bariatric Surgery (Gainesville, Florida) estimates that more than 15 million people in the U.S. suffer from morbid obesity and about 205,000 people are expected to have some form of bariatric surgery this year. A study published in the New England Journal of Medicine in August reported that morbidly obese patients who had bariatric surgery lost significant weight over the long term and are less likely to die from heart disease, diabetes and cancer within seven to 10 years following the surgery than those who did not have the operation.
Personalizing nutrition
The Foresight report, entitled "Tackling Obesities: Future Choices," is a two-year study that conducted in the UK by about 250 experts and scientist. It examined the causes of obesity and mapped future trends to help the government develop new health strategies.
The report predicted that more than half the population of Great Britain will be "extremely overweight" by 2050, resulting in an estimated cost of 45 billion for public health services and lost working hours.
The study identified nutrigenomics as a possible means for helping this situation by gaining an understanding of how nutrients and genes interact and how genetic variations can cause people to respond differently to food nutrients. This technology may enable consumers in the future to use personalized nutrition for determining which foods should be eaten. However, the study notes, there is a shortage of evidence regarding how successful this approach may be in achieving sustainable weight loss, particularly because there are more than 600 genes currently associated with obesity.
Dr. Clifton Bogardus and colleagues from the Diabetes Molecular Genetics Section of the National Institute of Diabetes and Digestive and Kidney Diseases (Phoenix), a unit of the National Institutes of Health, have identified a new obesity gene which is a variant of the ataxin-2 binding protein 1 gene (A2BP1) that was strongly associated with obesity in a native American population.
A growing problem: childhood obesity
In a welcoming message, C. Ray Nagin, mayor of New Orleans, wrote regarding the growing incidence of obesity that "we have now reached an alarming situation in which babies born today will probably live shorter lives than their parents."
Childhood obesity continues to expand in the U.S. and worldwide in developed countries. About 14% to 15% of all 15-year-olds in the U.S. are obese and about 22 million children under five years old are considered overweight. The National Health Nutrition Examination Survey was conducted during the period from 1976 to 1980 and again from 1999 to 2000. It found that the prevalence of overweight doubled among the 6-to-11 age group and tripled among the 12-to-17 age group.
Contributing factors are that food has become more affordable over the past few decades and has gone from nourishment to a source of pleasure in our society, featuring more food with empty calories. Recent studies also have implicated sedentary behavior and a dramatic increase in the intake of high-glycemic-index carbohydrates from carbonated drinks and juices as being leading causes in weight gain.
Overweight children are considered to be at an increased risk of coronary artery disease and Type 2 diabetes as they reach adulthood.
Hidden risks and pharmacology
Another potential complication of obesity in children and adolescents that often is overlooked is polcystic ovary disease, which is directly linked to obesity in women and to complications such as infertility. Also of great concern is the psychological impact that obesity may have on a child such as reduced self-esteem and social marginalization.
Jack Yanovski, MD, PhD, head of the Unit on Growth and Obesity of the National Institute of Child Health and Human Development (NIHD) of the NIH, gave a featured presentation on the use of pharmacologic agents for treating pediatric obesity, although there are no currently approved medications for obese children under 12 years old.
BMI may not be an effective measure of obesity in the pediatric population due to muscularity, rather than fat, which can influence the measurement.
Drug classes that can be used to control energy intake are noradrenergic (e.g., phentramine) and serotonergic (fenfluramine which was banned in 1997 due to adverse cardiovascular effects). Sibutramine is approved for use in children at least 16 years of age and is a combination of both these drug classes. Studies using these drugs were performed 15 to 20 years ago.
Orlistat, from GlaxoSmithKline (London), is the only approved drug for controlling energy expenditure in obese children of at least 12 years of age. It functions by breaking down triglycerides that reduces intestinal absorption.
Yanovski concluded that to be effective in weight loss, pharmacotherapy must be combined with lifestyle behavioral changes in diet and activity. He also briefly reviewed the use of bariatric surgery for pediatric patients and reported that both laparoscopic adjustable gastric banding and gastric bypass surgery resulted in clinically significant and sustained weight loss and stressed the need for vitamin supplementation after these procedures. Yanovski and his research team at NIHD reported that mutations in a gene called the melanocortin 3 receptor (MC3R) may cause children to eat more at meals. They found that children with two specific mutations in the gene weighed more and had more body fat than children with normal MC3R genes.
Adjustable gastric bands fill need
Allergan (Irvine, California) markets the Lap-Band system, which utilizes a saline-filled inflatable band that decreases the size of the gastric pouch, thus limiting the patient's ability for food intake. The band is connected to a percutaneous access port through which the surgeon may add or remove saline, adjusting the band's tightness and the size of the stoma. Its Omniform technology allows the Lap-Band System to maintain controlled, even and round inflation throughout adjustment range of the band.
Ethicon EndoSurgery (Cincinnati), a subsidiary of Johnson & Johnson (New Brunswick, New Jersey), received market clearance from the FDA in late September for its Realize adjustable gastric band for morbidly obesity adult patients having a BMI of at least 40 kg/m2, or a BMI of 35kg/m2 with one or more co-morbid conditions. The product is for use in patients that have failed more conservative weight-reduction alternatives, such as a supervised diet, exercise and behavior modification programs.
After implantation of the gastric band, a physician can inject or remove saline through a port attached to the abdominal wall to tighten or loosen the band.
The product is marketed outside the U.S. under the name Swedish Adjustable Gastric Band, where it has been sold since 1996 and used on more than 100,00 patients worldwide to help manage their weight.
Ethicon Endo-Surgery's other surgery product sold into this market is its Bariatric Edge Spiderman. It is a curved needle that is introduced through the esophagus and is used for stomach reduction. Competing products are G-Prox from USGI (San Clemente, California) and Endocinch from C.R. Bard (Murray Hill, New Jersey).
Intragastric balloon design issues
Intragastric balloons for obesity are currently available only outside the U.S. They are efficacious but are hampered by functional issues related to their design, such as difficulty changing balloon volume once implanted, inability to determine the patient's optimum balloon volume and migration into the small intestine leading to bowel obstruction and surgery.
The leading product is the intragastric balloon system from Allergan. A saline-filled silicone balloon that is placed inside the stomach to limit food consumption, it is sold in Europe and Latin America.
Spatz FGIA (Jericho, New York/Ra'anana, Israel) is developing a non-surgical treatment for obesity using an intragastric balloon. Its Floating Gastrointestinal Anchor design avoids migration to the duodenum and makes it easier and safer to use than other balloon devices that have been sold used outside of the U.S. for more than 10 years. The company claims that it yields a 15 kilogram weight loss over a six-month period. The device is in animal trials and is expected to enter into human trials in the first half of 2008, with the CE mark to follow and sales in Europe before year-end.
Gastric bypass vs. gastric band
The most common bariatric procedures performed in the U.S. are gastric bypass and the gastric band, which are typically performed laparoscopically.
These two procedures were compared in a study conducted by Nancy Puzziferri, MD, assistant professor in the division of GI/endocrine surgery at the University of Texas Southwestern Medical Center (Dallas).
It used non-randomized and retrospective data from a study comprising 1,100 gastric bypass patients and 633 lap-banding patients. The selection of bypass vs. band was based on the patient/surgeon discussion. She reported that for patients undergoing the gastric bypass procedure, the initial weight loss occurred faster and the average weight loss was greater after 24 months, as compared to gastric banding.
Success was defined as a loss of at least 40% of a patient's weight. There was a higher attrition rate among gastric bypass patients than gastric band patients. Puzziferri also noted the number of lap-banding procedures is increasing.
David Provost, MD, also from the University of Texas Southwestern Medical Center, reviewed the criteria for selecting a bariatric surgical procedure for morbidly obese patients. The procedures included laparoscopic adjusted gastric banding (LAGB), gastric bypass (GB) and biliary pancreatic diversion (BPD), although he rarely performs the latter procedure which is accompanied by significant malabsorption of nutrients.
Key considerations in selecting candidates for bariatric surgery are the potential for weight loss, co-morbidity resolution (e.g., hypertension, diabetes, GERD, asthma and sleep apnea), complications and mortality, along with the patient characteristics, such as age, gender and surgical preference.
He reported similar success in weight loss and co-morbidity resolution for patients having either LAGB or GB procedures over a two-year period, but the rate of weight loss was faster with LAGB patients along with a higher risk of life-threatening complications from this procedure. GB is easier to surgically reverse than LAGB, but the patient should consider that these procedures are permanent.
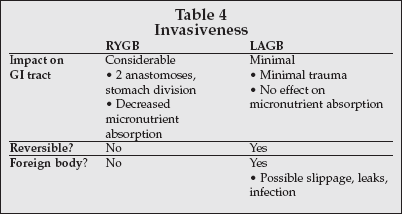
Provost also compared the Roux-en-Y gastric bypass (RYGB) open surgical procedure to LAGB laparoscopic gastric procedure as shown in Table 4.
 |
Implanted devices for weight control
EnteroMedics (St. Paul, Minnesota) is beginning a pivotal trial for Vbloc, a vagal blocking system for obesity control. The vagus controls gastric expansion of the stomach which occurs when food is consumed. The therapy is intended to circumvent this process and is delivered by laparoscopically implanting two leads adjacent to the vagal trunks just below the diaphragm. The leads are attached to a neuroregulator that is implanted — like a pacemaker — in a subcutaneous pocket. The product is intended for patients with BMI of 35 kg/m2 with a co-morbidity, or with a BMI of 40 kg/m2.
An advantage of this therapy over the bypass or banding procedures is that the patient can eat a normal diet. A paper presented by Michael Camilleri, MD, of the Mayo Clinic (Rochester, Minnesota), evaluated the Vbloc in 25 obese subjects and found that sustained vagal inhibition was achieved over a 12-week period.
StimPulse (Kiryat Shemona, Israel) is developing a sensing-and-stimulating implantable device that senses food intake into the digestive system and applies electrical stimulation to the digestive system in order to reduce the ability of further intake of food. Animal studies are under way, with fully implanted and integrated units that are wirelessly connected to a base unit to acquire signals from the digestive tract and to activate stimulation.
Behavior modification for weight control
MEND Central (London) exhibited and provided a poster of its program for achieving a measurable and sustainable reduction in child overweight and obesity levels. It is a government- and industry-sponsored free evidence-based and family oriented intervention program. It combines games that stimulate active enjoyment with learning about healthy eating and behavior modification techniques to boost self-confidence. MEND (Mind, Exercise, Nutrion ... Do it!) currently operates in England, Denmark and Australia. It is seeking sponsors to fund its expansion into the U.S.
BodyMedia (Pittsburgh) is distributing to clinicians its SenseWear WMS, a web-based weight management solution that focuses on behavior therapy. It consists of an armband for the automated tracking of activity and sleep, and is designed to improve weight loss outcomes by increasing patient adherence to prescriptions and promote lifestyle changes. It enables health practitioners and their patients to continuously monitor daily behaviors such as calories burned, nutrition and sleep.
Body composition analyzers
The number of exhibitors offering equipment for analyzing body composition has increased from prior years with the notable addition of the leading companies that market bone densitometers for monitoring osteoporosis, namely, Hologic (Bedford, Massachusetts) and GE Healthcare (Waukesha, Wisconsin). Body composition scans with dual-energy X-ray absorptiometry (DEXA) provides precise data on bone and tissue composition, including bone mineral density, lean tissue mass and fat tissue mass. These measurements help physicians monitor the effects of therapy, diet and exercise.
Cosmed (Rome/Chicago) featured its Fitmate equipment, which measures oxygen consumption in real time for determining resting energy expenditure for use in weight management, fitness assessment and exercise prescription.
Korr (Salt Lake City) displayed its ReeVue indirect calorimeter that measures the body's consumption of oxygen from a 10-minute breath test which is used to measure a patient's resting energy expenditure. This technique is used for nutritional assessment and medical nutrition therapy.
Tanita (Tokyo and Arlington Heights, Illinois) is a leading provider of precision scales.
Its WB-3000 digital beam scale features an automatic BMI calculation. Tanita uses bioelectrical impedance analysis which entails passing an electrical signal through the body which is carried by water and fluids. The impedance information is used to estimate the amount of lean and fat tissue within the body.
Tanita's MC-189 is a new body composition analyzer that uses four frequencies to generate a total body analysis which includes body fat, muscle mass and total body water along with detailed information on intracellular and extracellular water essential for fluid status and illness assessment.
Bodystat (Isle of Man, British Isles) markets bioelectrical impedance analysis equipment for measuring body fat, lean muscle, water content and BMI. Its single- and dual-multifrequency devices are used to determine intracellular and extracellular fluid levels.
