BBI Contributing Editor
Over the last two decades, there has been a continuing stream of changes in U.S. health care delivery, brought about by the movement away from fee-for-service medicine. We have seen shortened length of stay, growth in outpatient procedures and services, downgrading of provider skill levels, changes in quality, implementation of pathways and care maps, improvements in outcome tracking, and many other changes. It has been a climate in which medical suppliers have scrambled to accommodate the new paradigms in which health care is being delivered in the U.S. market. Companies that have not been nimble have suffered a bit, and those that have been nimble, have grown as a result. This culminated in the buying frenzy of 1999 — the Y2K year.
One would think that this rate of change could not continue, but we believe it will continue and accelerate during the first two decades of this millennium. Vendors must be aware of the drivers of this change in order to design products that will offer an attractive value equation to the administrators and caregivers of this evolving market. More than in the past, equipment vendors must understand the medical and administrative drivers of U.S. health care delivery and design products that offer real advantages compared to their competitors. Vendors also must do a much better job of understanding the basic dynamics of their markets — things like the aging of their installed base, the demographics of the hospitals that comprise their market and how the changes in medical and nursing paradigm will affect their market positions. Moreover, this knowledge must be empirical, not rhetorical, in its detail, in order to specify the right products, properly position sales resources and train personnel.
Many forces drive medical device markets
There are several key forces driving U.S. health care. Some are already apparent, such as reducing cost and length of stay while sustaining or improving quality. Others are new, among them the tidal wave of nursing shortage that is on the horizon and will soon crash ashore. Others are yet to come but inevitable, like the growth in need for beds and facilities as the U.S. population ages. Taken together these drivers set the stage for devices that offer new value equations and embody new technologies. Vendors that are responsive and nimble will see dramatic growth and profits. Those that are too slow (or too fast) will miss the wave of change and be left off-shore.
Demand for short-term hospital beds
Given the aging of U.S. population, at some point the long-established trend in the decline of staffed, short-term-care U.S. hospital beds will reverse. Indeed, it may have just done that. Consider the American Hospital Association (AHA; Chicago, Illinois) figures for the last five years (Table 1). Note that in spite of the decline in hospitals in 2000, the decline in staffed, short-term beds stopped.
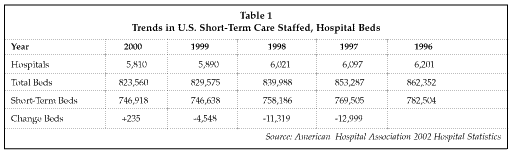 |
Whether the inflection point achieved in 2000 will continue in 2001 and later years will require some time to determine, but the deceleration in the decline of beds over the last five years, in spite of the reduction of total hospitals, is quite interesting. It is clear that within the next five to eight years we will reach an inflection point and the number of beds (and perhaps hospitals) will begin again to increase. This is a positive long-term trend for medical equipment suppliers, as each of these beds will ultimately become a monitored bed.
Aging drives growth in demand
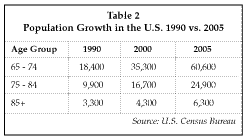
In 1990, citizens over age 65 made up about 13% of the total population in the U.S., according to Census Bureau data. By 2000, at the end of our forecast period, age 65 and older citizens will increase by only 1%. By 2010, the percentage of older citizens will increase by an additional 1% but thereafter climb remarkably. The numbers in Table 2 indicate the elderly population growth during the forecast period. Notice the rate of growth, which also will imply a growth in the demand for services for diseases associated with aging. This suggests that there will have to be some modest expansion in medical devices starting at the end of the survey period, and also that occupancy will rise. Those in the oldest group (85+) make the greatest demands on the health care system, but fortunately they do not rise as rapidly as the growth of the younger/old group.
 |
Developing nursing supply crisis
Another dramatic trend that will impact the medical device markets is the crisis in nursing availability. This is already manifesting itself, with 124,000+ unfilled positions for registered nurses. At the 2001 American Association of Critical Care Nurses (AACN; Aliso Viejo, California) meeting, projections of the nursing shortage reported were 794,000 by 2008. By 2020 the proportions of the shortage will be dramatic as the number of retired and aging Americans demanding care will have resulted in more beds being opened, while accelerating the shortage of registered nurses to staff them.
There is a growing shortage of qualified RNs for ICU positions in hospitals. The average ICU nurse is 47 years old, and three times as many RNs are leaving active hospital jobs as are entering the field. This is expected to continue over the forecast period, resulting in an acute shortage in the period from 2006-2015. Nursing salaries are expected to increase to attract candidates, and this will drive up hospitals' direct labor costs, further complicating their net profit situation.
Without fundamental changes in working conditions and wages, the shortage will reach the level of 20% within the next decade. At these levels of shortage, it is impossible to see how the quality of medical care in the U.S. will not be dramatically compromised.
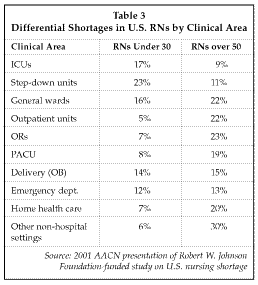
Table 3 shows the specific clinical areas in the hospital and in alternate sites where the percentage of older nurses (likely to retire or leave nursing in the next five to 10 years) will create the largest shortage of RNs.As shown in Table 3, the alternate site (non-hospital) sector, including home health care, plus the operating room, outpatient areas, PACU, OB/delivery, ER and general wards will be the sites of the greatest shortage of registered nurses in the near future. Only ICU and step-down units currently have more young nurses than older ones. This implies that hospitals will face a severe shortage of RNs that will span the majority of the hospital.
 |
Patient monitor design changes
The implication for medical device vendors is that the staffing of clinical areas that currently have monitors, as well as areas like general wards that currently do not have monitors, but will in the future, is likely to be with more licensed practical nurses (LPNs) and fewer RNs (presumably supervising them). These personnel will be less "monitor aware" and less able to recognize problems that the more educated and experienced RNs would normally recognize. They will also be less familiar with what to do when they do recognize a problem.
This is only one implication that the RN shortage will have on equipment design. Another is the entire setup of monitors for a clinical area. Monitors have evolved to the point that a setup can be predefined and stored in a user-accessible key of the monitor. Fukuda Denshi (Tokyo) implements such user-defined setups, but even this is less than required in the future. The setups needed for each clinical area should not only be predefined, but also automatically implemented without user intervention when the monitor is activated in any clinical area. Siemens' (Danvers, Massachusetts) "smart" docking station is an implementation of this concept and represents a prototype of this concept. The docking station configures any monitor that is attached to it for the parameters, alarm limits, etc. appropriate for monitoring in that clinical setting. This could also be done by storing the configurations in a central repository at "central station" or in a network-based repository, and then sensing new node activation and downloading the appropriate configuration into the monitor attached to the node. Such concepts of automatic configuration by clinical area are foreign to the design of most patient monitors offered today but will become standards for all monitors used in the next five years.
Future monitor configurations
Tomorrow's monitors will depart from the configuration offered by today's market leaders. The U.S. market leader is Philips Medical Systems (Andover, Massachusetts), through last year's acquisition of Agilent Technologies. Its current product line is fundamentally a stationary modular system. More recently, Philips has evolved to a portable, modular system augmented by a series of portable, configured, lower-acuity monitors. In the future, all monitors will be portable and networked. This will require a wholesale replacement of products available from some leading companies but less change for other suppliers who have already recognized this trend and responded to it. Again, Siemens offers the early prototypes of this transformation in its "pick-and-go" system of essentially two monitors — one modular and one configured, both portable and networked (either by cable or wirelessly).
Monitoring vendors will need to understand the proper mix of these types of products in order to present the best value equation to the hospital in the future, an understanding based on hard data, not rhetorical product management speculations or sales mix based on a single vendor's current products.
Where is the market?
The evolution of the hospital of the future will challenge current assumptions about where the market is. It will be important to determine how many units are represented by different size hospitals across all clinical unit segments. Take operating rooms, for example. What size of hospitals need to be covered to compete for 33%, 50%, 66% of the available business? Not many vendors can answer such questions accurately, but they will need to have such information to properly position their sales assets to compete for this business. Sources of such information are scarce; however, they are available from Medical Strategic Planning's (Lincroft, New Jersey) Reality Market Intelligence System.
In the largest hospitals, there can be up to 150 operating room suites. However, we have only plotted in Table 4 the distribution above up to units of 50 ORs, since this accounts for more than 98.3% of all operating suites in U.S. hospitals. The size of ORs is somewhat different than other clinical areas, in that there is a fairly even distribution from hospitals operating six to 12 ORs, and then a secondary relatively even distribution for hospitals having 14 to 24 ORs. Peaks thereafter exist at 30, 35, 40 and 50 ORs. Table 5 shows how these are distributed by the size of the hospital (staffed beds).
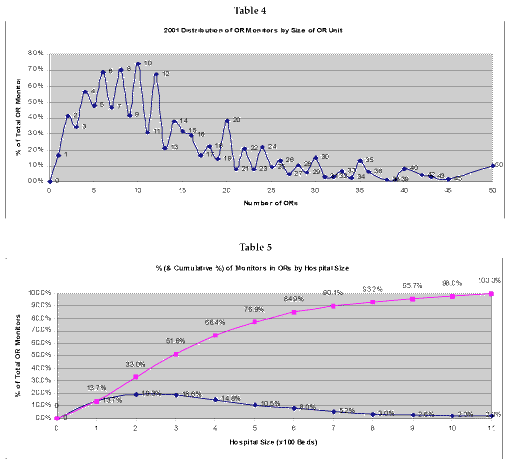 |
This shows that a vendor can access 33% of the available business by covering hospitals of 200 or fewer beds, and can extend their reach to 50% of the operating room business by covering hospitals of 300 beds. Two-thirds of the U.S. market can be competed for by covering hospitals of 400 or less beds, and three-fourths by covering hospitals with 500 or less beds. This flies against the conventional wisdom that a vendor needs to cover the larger hospitals and university settings to obtain access the majority of the U.S. market.
Indeed, in designing products for larger hospitals and university OR settings, which handle the most complex surgeries and are staffed with residents and interns, the product requirements incorporated may represent a poor value equation for the smaller hospitals in which the majority of the unit market resides, and may even be a misfit due to the staffing of such hospitals, which will be devoid of the intern and resident care givers (that somewhat mask the RN shortage in larger institutions and educational settings).
The size of the hospital and its relation to market potential varies from clinical unit to unit and by type of hospital (general, pediatric, women's, university, military), and a vendor needs to be aware of such variations to develop future monitors with the proper capabilities. The vendor's marketing organization also needs to be aware of such variations, particularly if they are small and have only a limited number of salesmen, to know which hospitals to call on and which to ignore.
Implication on architectural design
The intensive care unit of the future (and to the degree renovated ICU space allows, renovated ICUs) will increasingly adopt new designs to better support nursing activities with higher patient-to-RN ratios. This has implications for the room design and the design of other areas in the ICU. In the future, there will be a movement to ceiling mounting of equipment support columns to facilitate their repositioning to various locations around the patient's bed. These are coupled with mobile base columns, which double as bed transporters.
This concept is embodied in the new Hill-Rom EpiCare Porter product. EpiCare Porter leaves room around the patient where needed, including access to the head of the bed when necessary. It also leaves other space available in the room, allowing the room to be more "home" and less hospital-like. This also provides flexibility in the location of the bedside monitor, particularly if the monitoring system includes an infrared remote control, and permits the room to adapt to divergent care needs as patient and unit priorities change.
Distributed alcove observation pods
A more fundamental change is occurring in the notion of the "central station." In newer hospital unit designs, there isn't one central station — rather, there are several alcove-based mini-stations, up to one for each two to four rooms. These alcoves provide charting and surveillance locations for the nurses responsible for each patient, allowing the nurse to work closer and in view of the patients. Unit sizes are affected as well. ICUs with fewer than six beds will become even less cost-effective. Optimal size currently is eight to 10 beds, depending on the size of the rooms.
Newer units have larger rooms, shifting the number of rooms down to eight beds per ICU. It is possible to squeeze up to 10 beds per unit; however, doing so may sacrifice room size, which is not consistent with the design trend. Locating nursing alcoves between rooms uses up unit space as well, reducing the number of beds per unit within the 5,000-square-foot fire regulation limitations.
The "ideal" patient monitoring system of the future will be substantially, perhaps fundamentally different from the majority of products offered today. The user of these devices will be different, as will the delivery of care and the physical setting in which they are installed. Savvy vendors will anticipate and profit from these changes. Those who lag behind will suffer.
